Uterine fibroids are small tumors that develop in and around the walls of the uterus. The symptoms of fibroids can range from non-existent to debilitating pain depending on the size, location, and quantity of tumors.
Noncancerous in most cases, fibroids are incredibly common, with as many as 80 percent of women developing them by age 50. Uterine fibroids are typically diagnosed during routine gynecological check ups or secondary visits investigating symptoms.
Read on to learn the warning signs and symptoms of uterine fibroids as well as the current treatment options available.
What Are Uterine Fibroids?
Also called leiomyomas or myomas, uterine fibroids are growths made of smooth muscle cells and fibrous connective tissue. They may manifest alone or in clusters, ranging in size from as small as a grain of rice to as big as a watermelon, expanding the uterus to the rib cage.
Fibroids can grow on the outside of the uterus (subserosal fibroids), inside the muscle of the uterus (intramural fibroids), or into the uterine cavity (submucosal fibroids, the most rare type). They can also be pedunculated, or attached to the uterine wall by a stalk.
It’s not known what causes fibroids, although there are noted connections to ethnicity–African American women are diagnosed with fibroids at a higher rate than any other race–and estrogen production–fibroids contain more estrogen than typical uterine muscle cells and they typically shrink after menopause.
Learn more: What are uterine fibroids?
Transcript
Signs and Symptoms of Fibroids
Heavy Periods
One of the most common symptoms of uterine fibroids is abnormally heavy or long-lasting periods. For example, soaking through more than one pad or tampon every hour is considered abnormally heavy. Periods that last longer than six days are considered a symptom of menorrhagia, or heavy period, as well.
Pelvic and/or Abdominal Pain or Pressure
Chronic pain or discomfort in the pelvis or as high as the abdomen could be a sign of uterine fibroids, especially large fibroids that enlarge the abdomen. They may be causing a feeling of heaviness, bloating, or pressure that makes it uncomfortable to bend over or lie on your stomach.
Painful Sex
Large fibroids that develop near the cervix can cause mild discomfort, feelings of pressure, or even severe pain and bleeding during intercourse. Fibroids can also create a hormonal imbalance between estrogen and progesterone that can lower libido.
Low Back Pain
Low back pain with fibroids is caused by pain radiating from the pelvis, where the fibroids are pressing against organs. In rare instances, a large fibroid on the back side of the uterus may press against the nerves and muscles of the lower back, causing pain.
Constipation, Difficulty with Bowel Movements, and Rectal Pressure
Fibroids putting pressure on the bowel and/or bladder can cause incontinence, frequent urination (a common issue), the inability to urinate, and constipation. (The iron supplements prescribed to combat anemia due to heavy bleeding caused by fibroids can also cause constipation). In rare cases, fibroids can create kidney dysfunction where fibroids press on the ureters (tubes that carry urine from the kidneys to the bladder).
Similarly, fibroids that press against the rectum can cause a feeling of rectal fullness, pain during bowel movements, or difficulty having a bowel movement. Chronic constipation can also lead to hemorrhoids: painful, inflamed veins located in and near the rectum that can cause bleeding during bowel movements.
Emergency Fibroid Symptoms
Although tens of thousands of women visit emergency rooms every year for symptoms of fibroids, most of these cases can be treated in a non-emergency setting. Clearly female patients are not receiving the information and/or diagnoses they need from their doctors to prevent painful symptoms from fibroids.
This is why receiving care from fibroid experts can be crucial to avoiding the pain and stress of symptomatic fibroids.
How Are Fibroids Diagnosed?
- Fibroids are often discovered during pelvic exams as the doctor manually checks the uterus and other internal reproductive organs for abnormalities. This may happen during a routine gynecological checkup if there are asymptomatic fibroids, or at a visit to investigate if the cause of symptoms you’re experiencing are consistent with fibroids.
- Typically an ultrasound is then used to confirm the presence of fibroids, as well as their size and location. This may be an abdominal ultrasound, similar to a pregnancy ultrasound, or a transvaginal ultrasound, in which a small probe is inserted into the vagina.
- If there are multiple fibroids, ultrasounds can be ineffective at identifying their size and position. In cases like these, another diagnosis method such as saline sonography (Saline Infusion Sonohysterogram) may be used. A saline sonogram uses sterile saline injected into the uterus through a catheter to highlight any abnormal masses. This can provide a better picture of the exact location(s) of the fibroids and whether it could complicate pregnancy.
- An MRI is commonly used for women approaching menopause (or those with a larger uterus) to reveal in more detail the size and location of fibroids. An MRI is also necessary for women opting for uterine fibroid embolization treatment.
- Finally, hysteroscopy is a valuable tool for evaluating fibroids in women experiencing both menstrual issues and infertility. The doctor inserts a small, lighted telescope through the cervix into the uterus, then injects saline into the uterus, allowing them to both see and remove, if necessary, the fibroids from inside the uterus.
Do I Need to Get Fibroids Treated?
Treatment is not always necessary. If you are asymptomatic, once the fibroids are confirmed by testing to be benign, often nothing further needs to be done.
However, you should seek treatment if fibroids are negatively affecting your quality of life and/or causing excessive bleeding, pain, or bladder problems.
How Are Fibroids Treated?

Lifestyle changes are the simplest and cheapest way to improve your symptoms, whether you ultimately need further treatment or not. Eating healthy foods, such as those on the Mediterranean diet (e.g. whole grains, vegetables, fish, fruits, nuts), and reducing processed foods, alcohol, sugar, and caffeine can improve symptoms and keep fibroids from worsening. Exercising, managing stress, and taking supplements such as iron can all be beneficial, as well.
Medications are also a treatment option. Over-the-counter painkillers such as ibuprofen may be used for abdominal pain from fibroids, while birth control pills may be prescribed to help control heavy bleeding. Medications called gonadotropin-releasing hormone (GnRH) agonists can be used temporarily to shrink fibroids before surgery, but not long-term as they can lead to irreversible bone loss.
Surgery is a treatment method for fibroids that includes the removal of the fibroids (myomectomy) or the entire uterus (hysterectomy). But for the many patients who prefer to avoid major surgery, uterine fibroid embolization (UFE) is an alternative.
A minimally invasive endovascular intervention, UFE allows you to preserve your uterus and usually your fertility and doesn’t result in unsightly scarring.
VasCare Provides Diagnosis and Treatment in Corpus Christi and South Texas
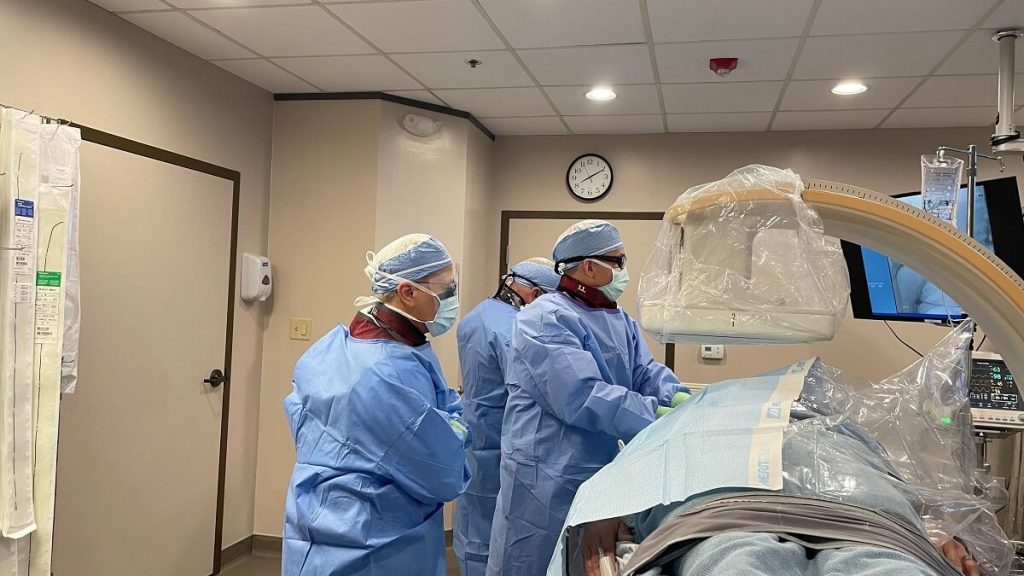
As leading UFE practitioners, we have seen the benefit to women of minimally invasive treatment with low risk of complications and a short recovery time.
If you’re experiencing fibroid symptoms in South Texas, come see us and hear how this exciting treatment can restore your quality of life.